Hip Cartilage Damage: Symptoms and Arthroscopic Treatments
Hip cartilage damage is a serious orthopedic issue that can lead to permanent joint stiffness and osteoarthritis if left untreated.
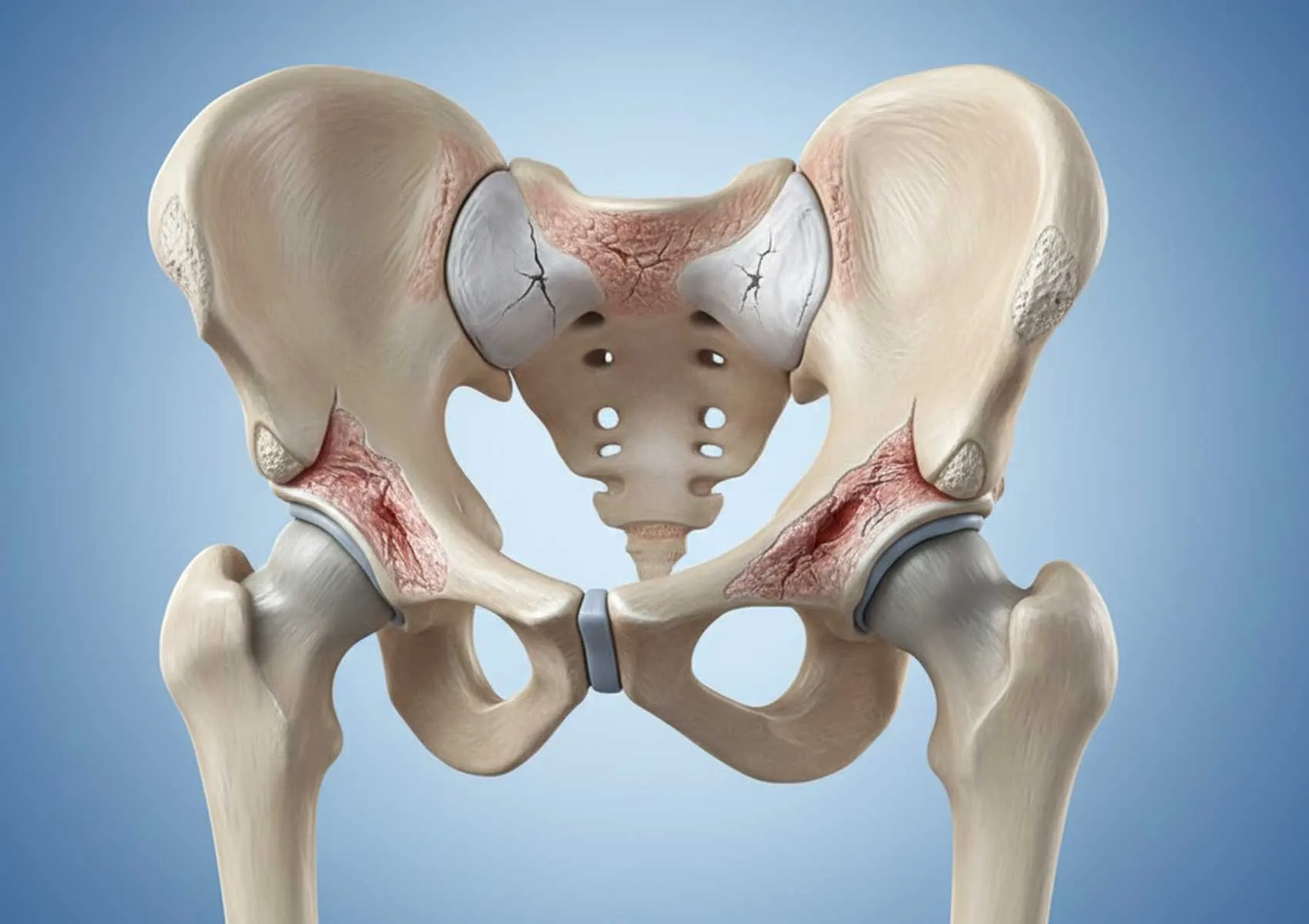
The hip joint is one of the largest weight-bearing joints in the body and is subjected to significant mechanical stress during daily activities. The smooth cartilage covering the joint surface is essential for pain-free and fluid movement. However, trauma, structural abnormalities, or gradual wear and tear can lead to hip cartilage damage. This condition causes complaints such as pain and restricted movement, reducing patients' quality of life.
When cartilage damage is diagnosed early, it can be managed with treatments aimed at preserving the joint, while more advanced cases may require comprehensive surgical interventions. This problem is especially significant among active individuals and athletes and should be managed with an appropriate treatment plan. This article will examine the causes, symptoms, and current treatment options for cartilage damage in detail.
What Is Hip Cartilage Damage?
Hip cartilage damage refers to the disruption of the hyaline cartilage that covers the joint surfaces between the femoral head and the acetabulum of the pelvis. In a healthy hip joint, cartilage allows bones to glide over each other without friction and acts as a shock absorber. Because cartilage contains no blood vessels or nerves, it has a limited capacity to heal itself when damaged.
Cartilage damage can range from superficial softening to deep defects exposing the bone surface. This process is often associated with hip joint diseases. The size and depth of the damage are critical factors in determining the treatment approach. For more information, please visit our cartilage diseases page.
Symptoms and Diagnostic Process
Cartilage damage may initially progress silently, but symptoms become more apparent as the injury worsens. Patients commonly report a deep ache in the groin area. This pain can worsen after prolonged sitting, when standing up, climbing stairs, or during sports activities. Additionally, sensations of catching, locking, or clicking in the joint may occur, possibly related to cartilage fragments within the joint or labral tears.
A thorough physical examination is essential for diagnosis. The physician evaluates hip range of motion and pain-provoking positions. Definitive diagnosis and grading of the damage are made using X-rays and Magnetic Resonance Imaging (MRI). Contrast-enhanced MRI (arthro-MRI) is particularly sensitive for detecting fine cracks on the cartilage surface and associated labral damage.
Causes and Risk Factors
Multiple factors may contribute to the development of hip cartilage damage. Traumatic events (falls, traffic accidents, etc.) can cause acute cartilage tears, while repetitive microtrauma gradually wears down the tissue. One of the most common structural causes is Femoroacetabular Impingement (FAI) syndrome. In this condition, deformities of the hip bones cause abnormal friction on the cartilage during movement, leading to damage.
Additional risk factors include developmental hip dysplasia (a sequel of hip dislocation), obesity, and professional sports, which place excessive load on the joint. Untreated cartilage damage may progress over time into osteoarthritis, commonly referred to as hip arthritis. Therefore, early symptoms should be regarded as the onset of hip osteoarthritis and taken seriously.
Treatment Methods
Treatment of hip cartilage damage is tailored according to the patient's age, activity level, and the size and location of the lesion. The primary goals are to relieve pain, restore joint function, and slow the progression of osteoarthritis.
Non-Surgical Approaches
For early-stage and small cartilage lesions, conservative treatment is preferred initially. This includes pain relief and anti-inflammatory medications (NSAIDs), activity modification, and weight control. Physical therapy programs aim to strengthen muscles around the hip to reduce joint load. Intra-articular injections of lubricating fluids such as hyaluronic acid can provide symptomatic relief.
Hip Arthroscopy and Microfracture Technique
Surgical options are considered when conservative management fails or mechanical symptoms such as catching persist. Today, the most commonly performed procedure is hip arthroscopy. This minimally invasive surgery involves inserting a camera and thin instruments into the joint through small incisions to address damaged tissues.
During surgery, unstable and damaged cartilage fragments are removed (debridement). In areas with cartilage loss, the hip microfracture technique may be applied to stimulate new tissue growth by activating the bone marrow. This involves creating small holes in the cartilage-deficient bone surface to allow stem cell-containing blood to reach the area, promoting the formation of repair tissue (fibrocartilage). More information about this procedure is available on our arthroscopic cartilage repair page. If impingement is the cause of cartilage damage, arthroscopic FAI treatment can also be performed in the same session to address the underlying problem.
Cellular Therapies (PRP, Stem Cells)
Biological treatments have gained ground in recent years, either as adjuncts to surgery or standalone therapies, to support cartilage repair. Platelet-Rich Plasma (PRP) and stem cell applications aim to enhance the healing potential of the damaged area. PRP and stem cell treatments, especially when combined with the microfracture technique, can improve the quality of newly formed tissue.
Post-Arthroscopy Recovery Process
Successful outcomes depend as much on rehabilitation as on the surgery itself. The recovery protocol varies according to the procedure performed (simple debridement or cartilage repair). Patients who undergo microfracture may need to use crutches for 4-6 weeks postoperatively to avoid full weight-bearing on the operated leg, which allows the new tissue to form.
The physiotherapy program focuses on maintaining joint mobility and regaining muscle strength. Return to sports usually occurs between 4 to 6 months post-surgery. For detailed rehabilitation protocols, please refer to our article on post-cartilage damage rehabilitation.
Scientific Sources and Disclaimers
This content has been prepared based on current medical literature and data from international orthopedic associations. Key sources include:
- National Center for Biotechnology Information (NCBI)
- Mayo Clinic - Hip Pain and Conditions
- American Academy of Orthopaedic Surgeons (OrthoInfo)
Medical information is continually updated and each patient’s condition is unique. Therefore, online information cannot replace professional medical examination.
This content is provided for informational purposes only and does not constitute medical advice. Diagnosis, treatment, and rehabilitation processes are individualized and must be planned under the supervision of a qualified healthcare professional. For any health concerns, please consult a healthcare provider. The information on this site is not a substitute for professional medical examination. Do not delay seeking professional care based on the information provided here.
FAQ
-
What is hip cartilage damage and how does it occur?
Hip cartilage damage refers to the wearing, tearing, or thinning of the cartilage that covers the joint surface. It typically occurs due to aging, injury, overuse, or joint conditions such as femoroacetabular impingement.
-
What are the symptoms of hip cartilage damage?
Common symptoms include pain in the groin or hip area, limited movement, and sensations of catching or locking in the joint. Pain often increases after prolonged sitting or standing.
-
Can hip cartilage damage be treated without surgery?
Non-surgical treatments like physical therapy, pain relievers, injections, and lifestyle changes may be effective in early stages. However, advanced damage or mechanical locking usually requires surgical intervention.
-
What is hip arthroscopy and how is it used for cartilage damage?
Hip arthroscopy is a minimally invasive surgical technique performed through small incisions using a camera to access the joint. For cartilage damage, it can involve cleaning damaged cartilage, stimulating new cartilage growth with microfracture, or performing cartilage transplantation.
-
What is the recovery process after hip arthroscopy?
Recovery varies based on the procedure and extent of damage but generally involves physical therapy and gradual return to activity. Full recovery and return to sports can take several weeks to months. Follow your doctor's guidance carefully.