What Is PRP Therapy? Differences from Stem Cells and What to Expect
What is PRP treatment? It involves using platelet-rich plasma derived from the patient's own blood to promote healing.
Biological treatment methods for musculoskeletal disorders have increasingly become alternatives or complements to surgery in recent years. Among these, PRP (Platelet-Rich Plasma) therapy is one of the most talked about and frequently asked about options. So, what exactly is PRP therapy and what role does it play in orthopedic conditions?
PRP therapy involves processing the patient’s own blood to concentrate platelets—tiny blood cells involved in clotting—and injecting this platelet-rich plasma into damaged tissues. This approach aims to stimulate the body’s natural repair mechanisms and is especially common for sports injuries and joint osteoarthritis. It is important to understand that PRP is not a miracle cure, but a scientifically grounded biological support process, which helps manage expectations appropriately.
How Does PRP Work? Mechanism of Action
The principle behind PRP therapy is that platelets in our blood, besides their role in clotting, carry growth factors essential for tissue repair. By centrifuging the blood, the platelet concentration is increased, and when injected into the injury site, it amplifies healing signals.
Injected platelets release growth factors that initiate tissue repair, potentially increasing blood flow to the area and activating cellular activities. For a more in-depth technical explanation, see our article on The Scientific Basis of PRP Therapy. Scientific literature, including studies on PubMed, often explores the potential effects of PRP on tendon and cartilage healing.
Differences Between Stem Cell Therapy and PRP
Many patients confuse PRP with stem cell therapy. Although both fall under the umbrella of regenerative or biological treatments, their mechanisms and purposes differ significantly.
While PRP acts as a "signal" or "catalyst" to speed up an existing healing process, stem cells serve as the "building blocks" capable of transforming into different tissue types. For advanced cartilage damage, for example, stem cell therapy for cartilage injuries may be a more complex option.
PRP in Orthopedics: When Is It Used?
In orthopedic and trauma practice, PRP can be applied alone or as an adjunct to surgical repair. Its uses are broad but may not be suitable for every patient.
Common indications include:
- Tendon Injuries: Used to support healing in chronic tendon issues like tennis elbow and Achilles tendinitis. Detailed information is available on our PRP treatment for sports injuries page.
- Joint Osteoarthritis: Typically applied in early to moderate knee osteoarthritis to reduce pain and improve function.
- Ligament Injuries: Can be used for partial tears such as injuries to the medial collateral ligament (MCL) or to accelerate healing after anterior cruciate ligament (ACL) reconstruction.
- Hip Conditions: Supportive treatment for hip joint osteoarthritis or labral tears, with scientific studies on PRP effectiveness in the hip joint available.
Authorities like the American Academy of Orthopaedic Surgeons (AAOS) acknowledge that PRP may provide symptomatic relief in select cases but emphasize that its effectiveness varies among individuals.
What to Expect from PRP Therapy?
PRP is not an instant pain relief injection. Being a biological process, tissue repair requires time. It is crucial for patients to set realistic expectations.
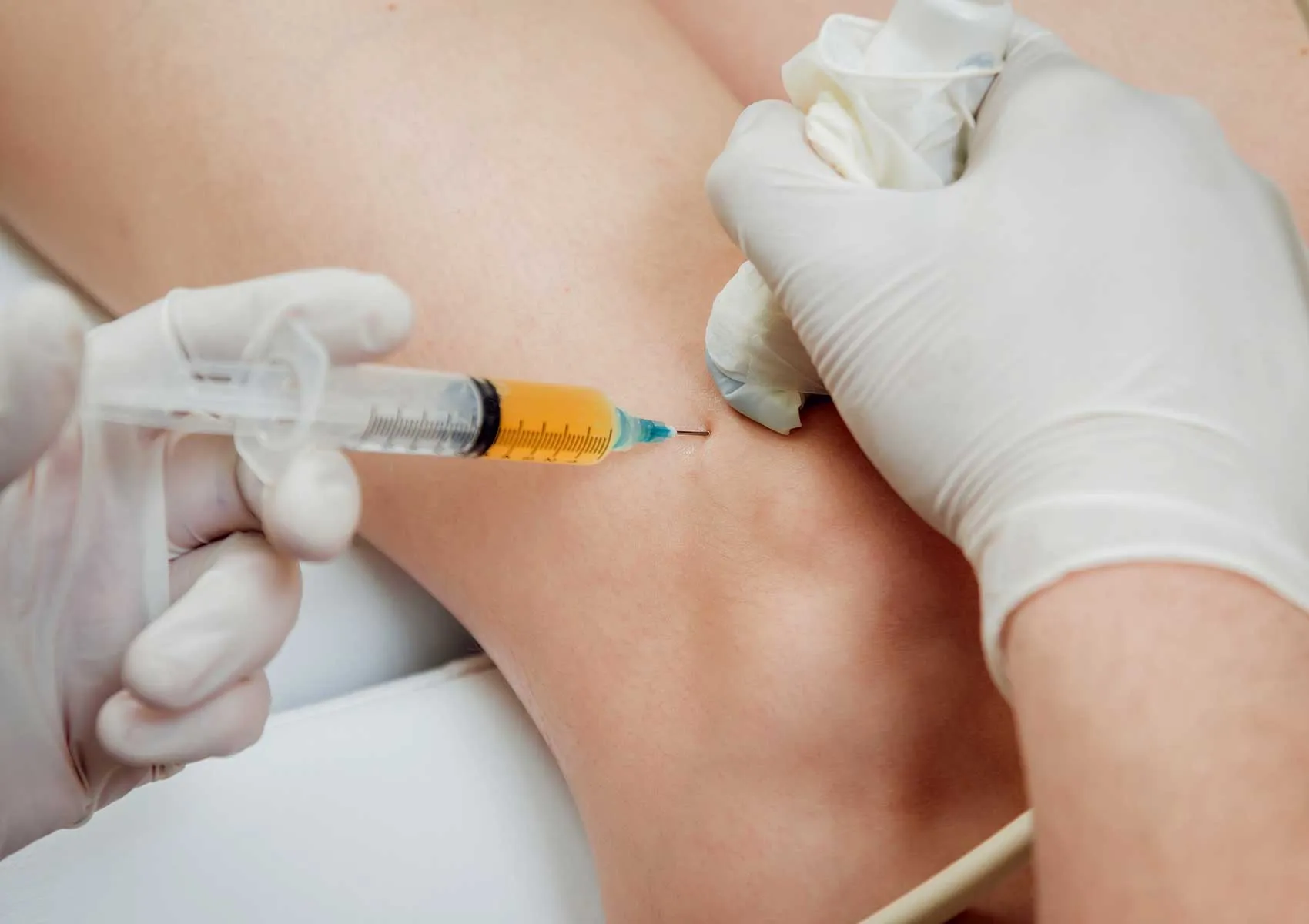
The procedure typically takes place in an outpatient setting and lasts about 30-45 minutes. Sterile technique is critical throughout. The image below shows an injection being administered by a specialist.
Some temporary increase in pain after treatment is common and considered part of the healing response. Signs of improvement usually begin within a few weeks. The duration for PRP effectiveness depends on the extent of damage and patient metabolism. For broader information on biological treatment options, please refer to our dedicated pages.
Risks, Limitations, and Suitability
Since PRP is prepared from the patient’s own blood, risks of allergy or tissue rejection are negligible. However, as with any injection, there are low risks of infection, nerve injury, or localized pain.
PRP is not suitable for everyone. It is contraindicated in cases of active infections, bleeding disorders, or certain cancers. In advanced cartilage diseases, PRP alone might be insufficient, and surgical options may need to be considered. Treatment decisions should always be made by a qualified physician based on clinical evaluation and imaging.
This content is provided for general informational purposes only and does not constitute medical advice. The information presented does not replace professional medical diagnosis or treatment. If you have any questions or concerns about your health, please consult a qualified healthcare professional. The author and publisher are not responsible for any outcomes resulting from the use of this content. Do not delay seeking medical care based on this information.
FAQ
-
What exactly is PRP therapy and how does it work?
PRP (Platelet-Rich Plasma) therapy involves injecting plasma rich in platelets, obtained from the patient’s own blood, into the damaged tissue. This process uses naturally occurring growth factors in the blood to accelerate healing and support tissue regeneration.
-
What are the main differences between PRP therapy and stem cell therapy?
PRP uses the patient's own platelets and growth factors from their blood, while stem cell therapy involves special regenerative cells that can transform into various cell types. Stem cells are typically used for more complex tissue repairs, whereas PRP mainly focuses on reducing inflammation and speeding up recovery.
-
In what cases is PRP therapy preferred and who is it suitable for?
PRP is commonly used for joint osteoarthritis, tendon injuries (like tennis elbow), muscle tears, and certain ligament injuries. Suitability depends on the patient’s overall health, blood test results, and severity of the condition, and should be determined by a medical specialist.
-
How long does PRP therapy take and what is the recovery process like?
The PRP injection procedure usually takes about 30 to 60 minutes. Full recovery time varies depending on the treated area and individual factors. Gradual improvement is typically seen within a few weeks. Following your doctor’s advice on rest and exercise after treatment is important.
-
What results or expectations should I have after PRP therapy?
After PRP therapy, you can expect pain reduction, improved function, and faster tissue repair. However, results vary between individuals, and instant miraculous recovery is not guaranteed. It’s important to have realistic expectations and discuss them with your doctor.