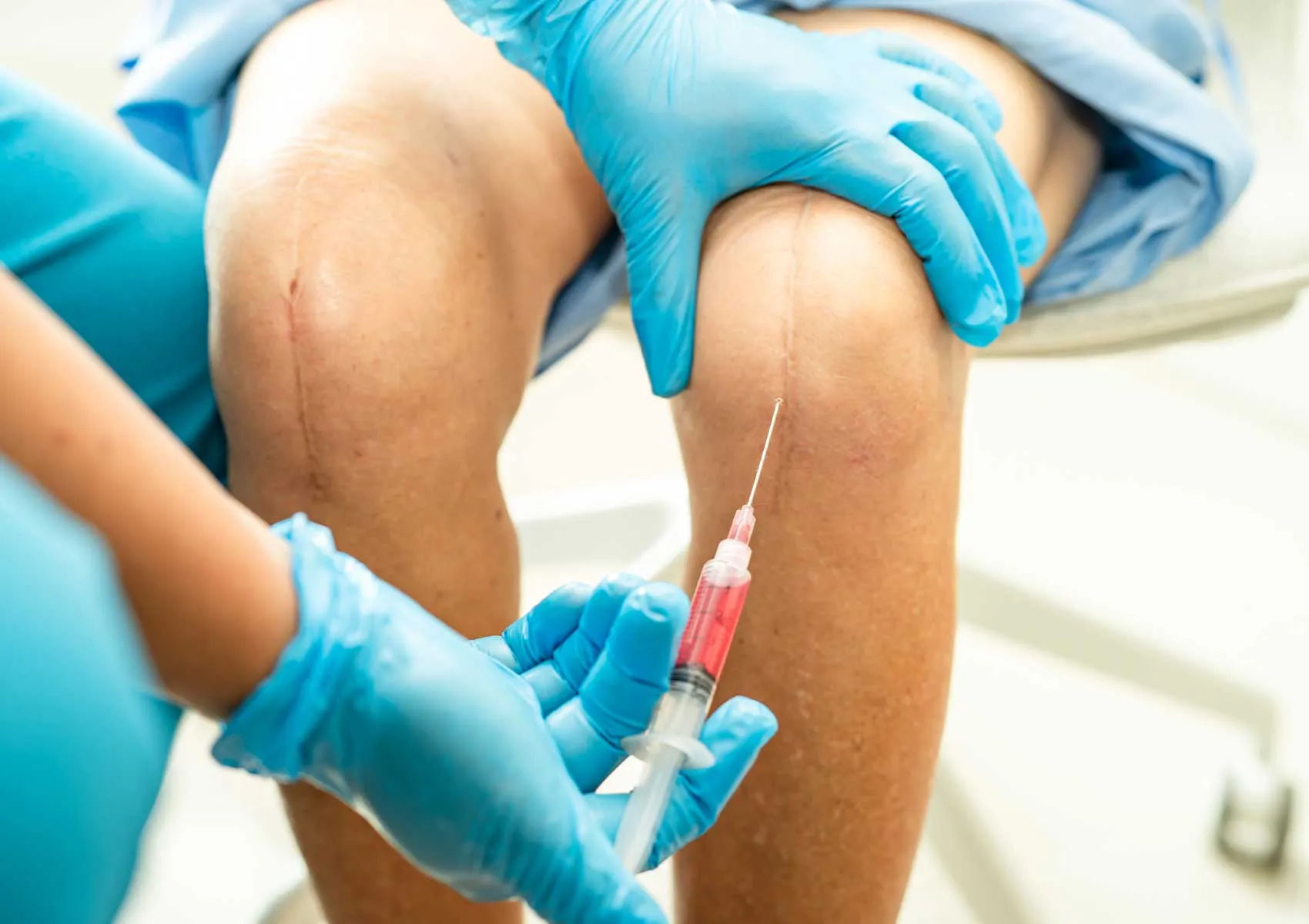
Stem Cell Therapy in Orthopedics: Facts and Applications
Stem cell therapy in orthopedics is a regenerative approach aimed at supporting the body's natural repair mechanisms to help heal damaged tissues.
With advances in modern medicine, regenerative treatments are gaining importance in musculoskeletal disorder management. Among these, stem cell therapy in orthopedics aims to leverage the body’s innate healing potential to support the repair of damaged tissues. This approach is utilized particularly in chronic conditions such as joint osteoarthritis, cartilage damage, and tendon injuries, offering a non-surgical alternative or adjunct to surgical interventions.
Stem cell therapy, introduced when conventional treatments fall short, relies on using cells derived from the patient’s own tissues. Part of cellular treatment methods, stem cell applications are designed to accelerate the biological repair process. However, as with any medical intervention, understanding the scientific foundations, indications, and limitations of this therapy is essential for proper expectation management.
What Are Stem Cells and How Are They Obtained?
Stem cells are undifferentiated cells forming the foundation of all tissues and organs in the body. In orthopedics, mesenchymal stem cells are primarily used—these can differentiate into cartilage, bone, muscle, and connective tissue cells. When introduced into injured areas, they contribute directly to repair and secrete signaling molecules that promote healing.
Orthopedic stem cells are typically autologous, harvested from the patient’s own body. The most common sources are bone marrow (usually from the pelvic bone) and adipose tissue from the abdomen. Bone marrow-derived cells have high potential for cartilage and bone repair, whereas adipose-derived cells are abundant and easier to harvest. The source is selected by the physician based on the patient's age, health status, and the specific condition to be treated.
How Is Stem Cell Therapy Applied in Orthopedics?
The treatment is performed under sterile conditions, generally with local anesthesia or sedation. It involves three key steps: collection, processing, and application of cells. Timing and technique precision affect the viability of harvested cells.
First, tissue is aspirated from the predetermined site using specialized needles. This sample undergoes centrifugation and filtration to concentrate the stem cells. The resulting preparation is then injected into the damaged area under imaging guidance such as ultrasound or fluoroscopy.
Which Orthopedic Conditions Are Treated?
Stem cell therapy is preferred for conditions involving tissue loss or degeneration. The most common use is osteoarthritis of the knee and hip, aiming to reduce pain and maintain joint function. It also shows promise in stem cell treatment in cartilage damage, particularly for focal cartilage defects in younger, active patients.
Additionally, it may accelerate healing in meniscal tears, rotator cuff injuries, and Achilles tendon problems. Early-stage avascular necrosis (bone blood supply disruption) is another indication when assessing hip joint diseases and treatment options. The diagram below marks the anatomical sites amenable to treatment.
Mechanism of Action of Stem Cell Therapy
The therapeutic effect of stem cells extends beyond their differentiation into damaged tissues. They exert significant effects through a "paracrine mechanism," releasing growth factors and anti-inflammatory cytokines that stimulate surrounding cells. These biological signals enhance local blood flow, prevent cell death, and initiate tissue repair.
This cellular-level process represents biological remodeling, potentially slowing disease progression while alleviating symptoms.
Differences Between PRP and Stem Cell Therapy
There is frequent confusion between prp treatment orthopedics and stem cell therapy, but they are fundamentally distinct biological approaches. PRP (platelet-rich plasma) is derived from blood and contains growth factors that aid healing but contains few or no live stem cells. Stem cell therapy delivers live cells capable of regeneration and differentiation.
When selecting among non-surgical joint treatment methods, disease severity guides the choice. PRP is generally reserved for mild injuries and soft tissue conditions, while stem cells may be considered for more advanced cartilage damage or osteoarthritis.
Potential Benefits and Risks of the Treatment
A major advantage of stem cell therapy is its autologous nature, minimizing risks of allergic response or tissue rejection. Being less invasive than surgery, offering outpatient treatment without hospital stays, and facilitating faster return to daily activities are additional benefits. Patients seeking pre-knee replacement alternative treatments may consider this option to delay surgery or manage symptoms.
Nonetheless, risks include temporary pain, swelling, and rare infections at the injection site. The efficacy varies per individual; not all patients achieve the same degree of improvement. Combining stem cell or prp support in sports injuries with arthroscopic surgery advantages and supportive treatments can enhance outcomes. The visual below symbolically illustrates tissue healing progression after treatment.
Scientific Sources and Medical Disclaimer
This article presents information based on current scientific research and clinical studies. Research into stem cell therapy in orthopedics is rapidly evolving, and treatment protocols are subject to ongoing refinement. Primary sources referenced include:
- PubMed (National Library of Medicine)
- World Health Organization (WHO)
- Mayo Clinic
- The New England Journal of Medicine (NEJM)
- OrthoInfo (American Academy of Orthopaedic Surgeons)
- ScienceDirect
This content is intended for informational purposes only and does not substitute professional medical advice, diagnosis, or treatment. Always consult your physician or a qualified healthcare professional regarding any health concerns. The information provided here does not constitute personalized treatment recommendations. Outcomes of regenerative therapies may vary from person to person and are not guaranteed. Do not delay seeking necessary medical care based on this content.
FAQ
-
What is stem cell therapy in orthopedics?
Stem cell therapy in orthopedics is a regenerative approach that uses the body’s own healing potential to repair damaged cartilage, bone, tendon, or ligament tissues. Typically, cells are harvested from the patient’s own body.
-
Which orthopedic conditions can be treated with stem cell therapy?
This therapy can be applied to conditions such as osteoarthritis of the knee, hip, and shoulder, meniscus tears, tendon injuries, and issues like tennis or golfer’s elbow. Suitability should be assessed by a specialist for each individual case.
-
Is stem cell therapy painful and what is the recovery process like?
The procedure is usually done under local anesthesia and may cause mild discomfort. Recovery varies from person to person but typically takes several weeks to months and can be supported with physical therapy.
-
Is stem cell therapy suitable for everyone and are there any side effects?
Stem cell therapy is not appropriate for every patient; factors such as age, overall health, and severity of the condition are important. Serious side effects are rare, but mild side effects like pain or infection at the injection site can occur. Always consult a specialist for detailed information before treatment.
-
How long does the effect of stem cell therapy last?
The effectiveness and duration of the therapy depend on the patient’s condition, the treated area, and the type of cells used. Some patients experience long-lasting relief, while others may need additional treatments. Scientific research in this area is ongoing.