Hip Joint Disorders: Causes, Symptoms, and Treatments
Hip joint diseases encompass various conditions such as arthritis, femoroacetabular impingement, and labral tears, with accurate diagnosis being crucial for an effective treatment plan.
The hip joint is one of the largest and most mobile joints in the body, playing a vital role in essential functions such as walking, running, and sitting. However, various factors can cause problems in this joint, significantly affecting quality of life. Hip joint disorders may lead to pain, reduced range of motion, and functional impairment, making daily activities challenging. These conditions cover a broad spectrum, from age-related degeneration and traumatic injuries to congenital anomalies and inflammatory rheumatic diseases.
Early diagnosis and an accurate treatment plan are critical for preserving hip joint health and preventing progressive damage. Modern medicine offers advanced imaging techniques for diagnosis, while treatment ranges from conservative methods to minimally invasive surgery. This comprehensive guide provides detailed information on hip joint disorders, covering causes, symptoms, diagnostic procedures, and current treatment approaches.
Hip Joint Anatomy and Function
Understanding the complex structure and function of the hip joint is a fundamental step in grasping the causes of hip diseases and their treatment methods. The hip is a ball-and-socket joint designed to provide both stability and a wide range of motion.
Structures Within the Hip Joint
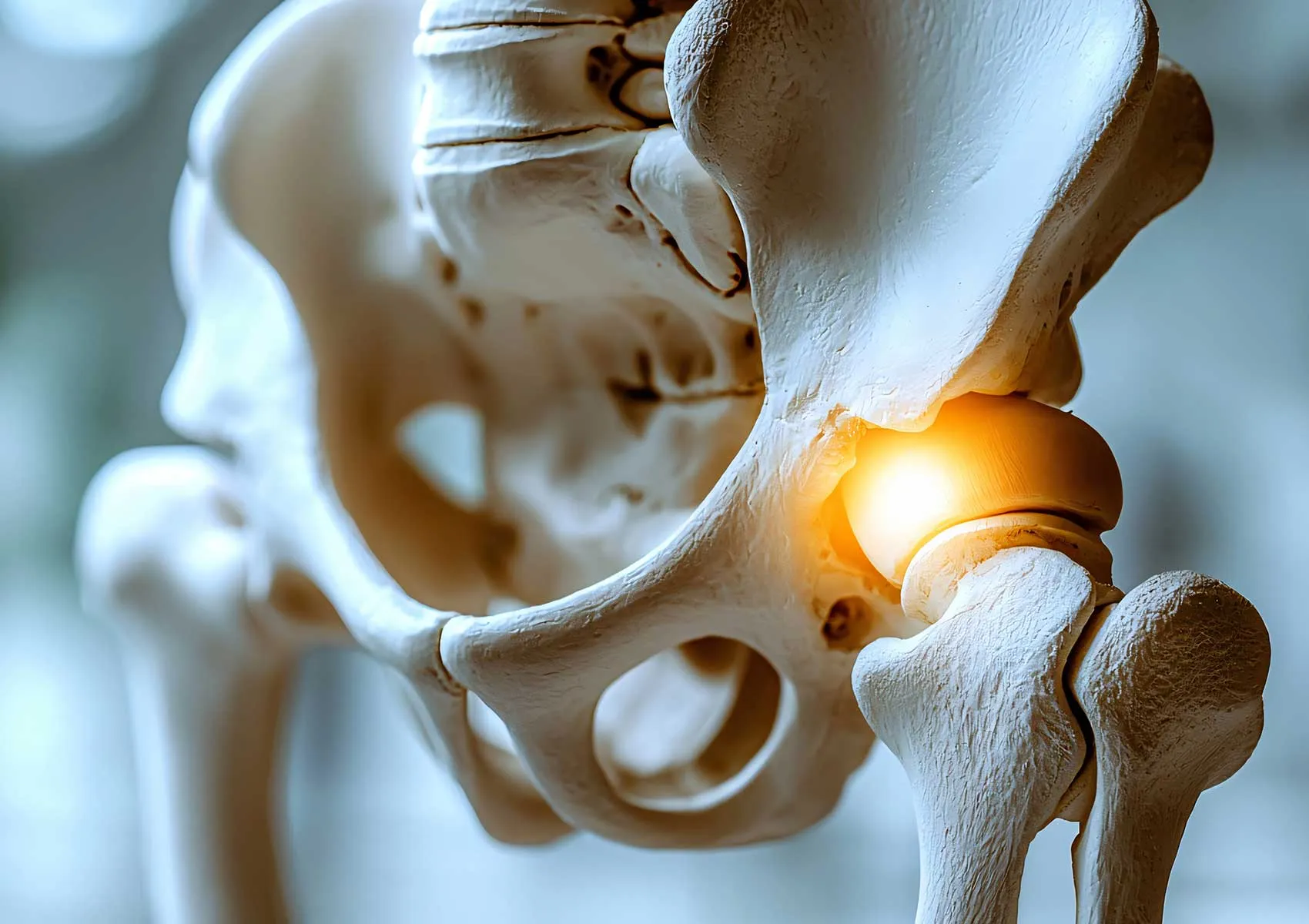
The hip joint consists of the head of the thigh bone (femur) fitting into the socket (acetabulum) of the pelvic bone. These two bone surfaces are covered with articular cartilage, which reduces friction and allows smooth movement. Surrounding the acetabulum is a ring of cartilage called the labrum, which enhances joint stability and helps keep the synovial fluid in place. Strong ligaments, tendons, and muscles surrounding the joint provide support and enable movement of the leg in various directions.
Factors Leading to Impaired Hip Function
The healthy function of the hip joint depends on the harmonious interaction of these anatomical structures. However, several factors can disrupt this balance, causing loss of function and pain. These factors include age-related cartilage wear (degeneration), sports injuries or accidents (trauma), congenital structural abnormalities, overuse, and inflammatory rheumatic diseases. Such factors can lead to cartilage damage, labral tears, or changes in the bone structure, setting the stage for the development of hip joint disorders.
What Are Hip Joint Disorders?
There are numerous diseases that affect the hip joint. Accurate identification of these diseases is essential in determining the appropriate treatment strategy.
Osteoarthritis and Rheumatoid Arthritis
Osteoarthritis is one of the most common causes of hip joint disorders. It involves the gradual wear and tear of the joint cartilage. This leads to bone surfaces rubbing against each other, causing pain, stiffness, and loss of movement. Rheumatoid arthritis is an inflammatory disease in which the immune system attacks the joints. In the hip, this can cause inflammation, swelling, and progressive damage.
Femoroacetabular Impingement (FAI)
Femoroacetabular Impingement (FAI) occurs when abnormal bone formation on the femoral head or the acetabulum causes abnormal contact and friction within the joint. It is especially common among young, active individuals and can cause pain during movement, along with cartilage and labral damage over time. FAI is divided primarily into “Cam” and “Pincer” types, and sometimes both occur simultaneously. Treatment of Femoroacetabular Impingement is planned according to symptom severity and the extent of joint damage.
Labral Tears and Bursitis
Labral tears refer to damage to the cartilage ring surrounding the acetabulum. This can result from trauma, FAI, or repetitive strain. Symptoms include locking, catching sensations, and deep groin pain. More details can be found in the source on hip labral tears. Bursitis is the inflammation of fluid-filled sacs called bursae around the joint. It often causes pain on the outer side of the hip and is associated with overuse or trauma.
Causes and Symptoms of Hip Pain
Hip pain is the most common symptom of hip joint disorders but may not always originate directly from the joint. As Johns Hopkins Medicine notes, problems originating from the back, spine, or pelvis can also cause referred pain in the hip region. Common symptoms include:
- Pain felt in the groin, hip, or thigh
- Joint stiffness, especially in the morning or after periods of rest
- Difficulty walking, climbing stairs, or bending
- Reduced range of motion in the joint
- Locking, catching, or clicking sounds during movement
- Limping while walking
The severity and type of symptoms vary depending on the underlying disease. Persistent hip pain should always be evaluated by an orthopedic specialist for accurate diagnosis.
Diagnostic Methods for Hip Joint Disorders
Correct diagnosis of hip joint diseases is the first and most important step in effective treatment planning. The diagnostic process usually involves multiple stages. Initially, the physician collects detailed patient history and asks about symptoms (pain location, onset, activities that worsen it, etc.).
Next, a physical examination assesses hip range of motion, stability, and tenderness. The physician uses specific tests to identify the pain source. To support clinical findings and visualize joint structures, various imaging modalities are employed. X-rays are fundamental for showing bony changes, fractures, or signs of arthritis. Magnetic Resonance Imaging (MRI) offers a more detailed view of soft tissues such as the labrum, cartilage, and tendons, providing valuable information for diagnosing conditions like FAI, labral tears, or avascular necrosis.
Treatment Options for Hip Joint Disorders
Treatment depends on the underlying cause, disease stage, patient age, and activity level. Approaches are generally divided into conservative (non-surgical) and surgical methods.
Medication and Physical Therapy
Conservative treatments are usually the first step. Anti-inflammatory medications can help control pain and inflammation. Physical therapy plays a crucial role in strengthening muscles around the hip, improving flexibility, and restoring joint mobility. Therapy programs include personalized exercises and manual therapy techniques. Intra-articular injections (such as corticosteroids or hyaluronic acid) may also provide temporary symptom relief. These methods are commonly considered in cases such as cartilage disorders.
Joint-Preserving Surgical Techniques
Joint-preserving surgery aims to restore function while maintaining the natural anatomy of the hip. This approach is often preferred for younger, active patients to delay or avoid total hip replacement. In conditions like FAI or labral tears, arthroscopic procedures shave down bone spurs or repair damaged tissue. Additionally, biological treatments such as Platelet-Rich Plasma (PRP) can support healing and enhance recovery when combined with surgery.
Arthroscopic Procedures and Joint Replacement Surgery
Arthroscopic surgery is a minimally invasive method performed through small incisions using a camera and specialized instruments. Hip arthroscopy is used for labral repair, correction of FAI deformities, and removal of loose cartilage fragments. This technique offers faster recovery and less pain. For advanced cartilage damage and severe arthritis, total hip replacement surgery is considered. This procedure replaces damaged joint surfaces with implants made of metal, plastic, or ceramic. Surgical candidacy is determined by factors such as the patient’s general health and extent of joint damage, as described in criteria for knee and hip replacement.
Post-Treatment Rehabilitation and Supportive Care
Rehabilitation following treatment, whether surgical or conservative, is vital for achieving successful outcomes and enabling rapid return to daily activities. Rehabilitation is typically conducted under the supervision of an experienced physiotherapist and tailored to the individual.
Goals of rehabilitation include managing pain, restoring joint range of motion, strengthening muscles around the hip, and normalizing walking patterns. Especially in cases of sports injuries, rehabilitation principles provide a structured plan for safe return to activity. Biological treatments such as PRP may also support tissue repair. More information on PRP applications and its efficacy can help understand the potential benefits of this adjunct therapy.
Recommendations for Maintaining Hip Health
Adopting certain lifestyle changes can effectively protect hip joint health and reduce disease risk. These measures can alleviate existing symptoms and prevent future complications:
- Maintain an ideal body weight: Excess weight increases load on the hip joints and accelerates cartilage wear. Maintaining a healthy weight reduces joint stress.
- Regular exercise: Low-impact activities like swimming, cycling, and walking strengthen muscles without overloading the joints and improve flexibility.
- Posture awareness: Maintaining correct posture when sitting and standing helps distribute joint load evenly.
- Avoid high-impact movements: Individuals at risk should avoid sudden twisting, jumping, and other high-impact activities.
- Balanced nutrition: A diet rich in calcium and vitamin D supports bone health and indirectly benefits joint function.
Hip joint disorders can be managed effectively with early diagnosis and appropriate treatment. Ignoring symptoms and delaying consultation with a specialist may compromise long-term joint health.
The content provided on this website is intended for general informational purposes only and is not a substitute for professional medical advice, diagnosis, or treatment. Always seek the advice of your physician or other qualified healthcare provider with any questions you may
FAQ
-
What are common hip joint diseases?
Hip joint diseases include conditions like arthritis, labral tears, femoroacetabular impingement (FAI), bursitis, and avascular necrosis. These often cause pain, limited movement, and difficulties with daily activities. It is important to consult a specialist for accurate diagnosis and treatment.
-
What conditions can cause hip pain?
Hip pain can be a sign of osteoarthritis, rheumatoid arthritis, tendinitis, muscle strains, nerve compression, or hip fractures. Identifying the exact cause may require a thorough examination and imaging tests. Consulting an orthopedic specialist is essential for a precise diagnosis.
-
How are hip joint diseases diagnosed?
Diagnosis of hip joint diseases involves a physical examination, patient medical history, X-rays, MRI (magnetic resonance imaging), CT (computed tomography) scans, and sometimes blood tests. These help to assess the condition of the joint and any potential damage in detail.
-
How are hip joint diseases treated?
Treatment depends on the type and severity of the disease. Conservative treatments include medications, physical therapy, and injections, while advanced cases may require surgical options such as arthroscopy or total hip replacement. Always consult your doctor to determine the best treatment plan.
-
How can hip joint health be maintained?
Maintaining hip joint health involves regular exercise, keeping a healthy weight, using proper posture and movement techniques, avoiding heavy lifting, and ensuring balanced nutrition. If you experience any pain or discomfort, it is recommended to see a healthcare professional.