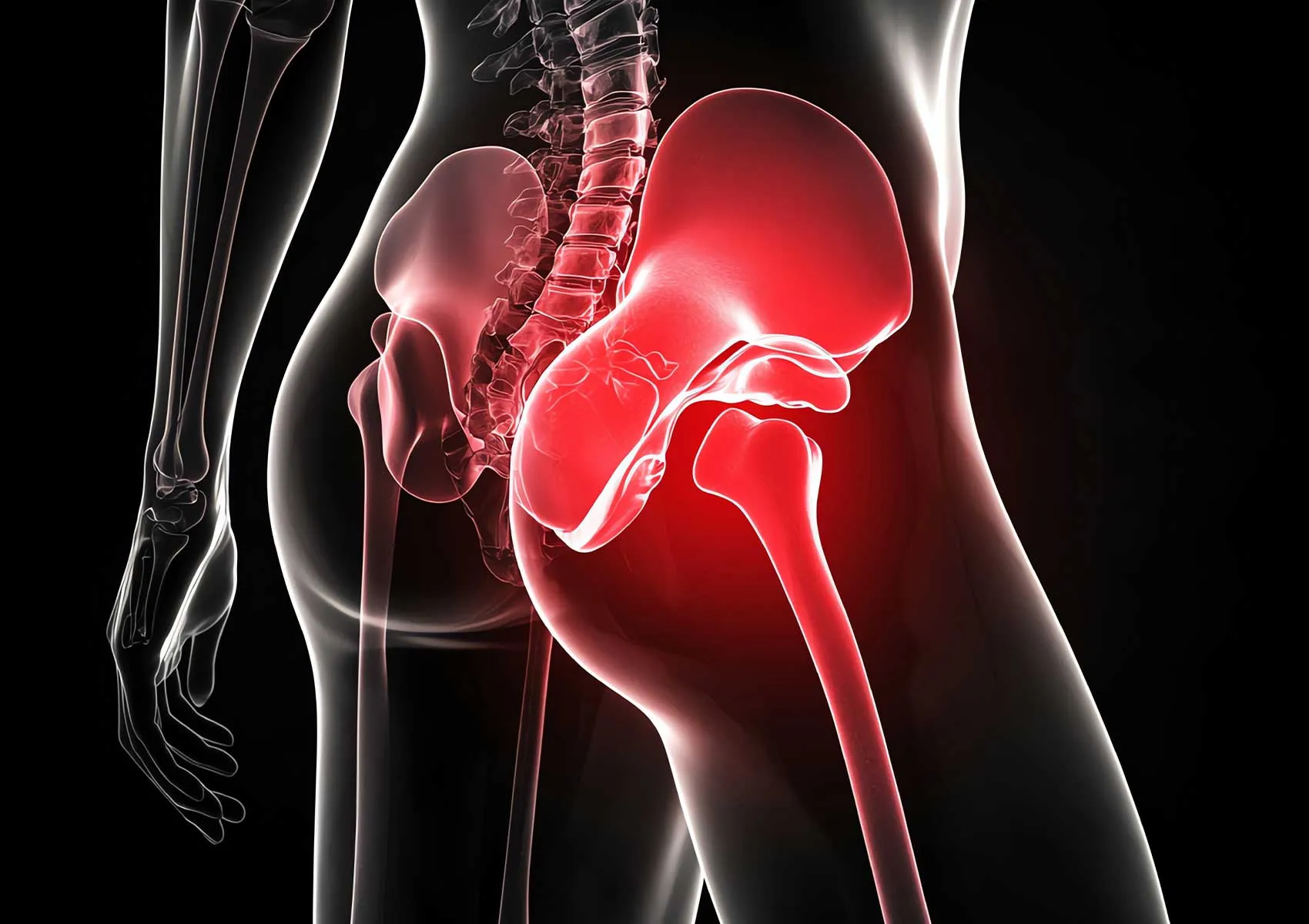
Hip Pain Causes: Arthritis or Impingement?
Common causes of hip pain include osteoarthritis and femoroacetabular impingement syndrome.
The hip joint is one of the largest load-bearing joints in the body, and its complex anatomical structure requires expert evaluation to identify sources of pain. The causes of hip pain range from simple muscle strains to arthritis, impingement syndromes, and referred pain. Pain felt particularly in the groin area is among the most common reasons patients seek medical help.
This guide will cover potential causes of hip pain, with a focus on differentiating between arthritis and impingement syndrome. The nature, triggers, and location of the pain offer the first clues toward an accurate diagnosis. However, definitive diagnosis and treatment planning require a comprehensive orthopedic examination.
What Is Hip Pain and Where Is It Felt?
Patients may describe hip pain in various regions, and the location is critical for the physician’s diagnosis. Differentiating pain originating from the hip joint itself from pain referred from surrounding tissues depends on understanding the anatomy.
For detailed anatomical information, you can visit Hip joint anatomy and what defines a healthy hip.
Common Pain Locations in Hip Pain
Where the pain is felt gives significant indications about the pathology. Patients often say "my hip hurts," but the pain may actually originate from the lower back, pelvis, or thigh.
Most Common Causes of Hip Pain
When examining patients in orthopedic clinics, mechanical issues and degenerative diseases surface as leading causes of hip pain. Having a general understanding of Hip joint diseases can help manage the process.
Hip Arthritis (Osteoarthritis)
Commonly referred to as arthritis, osteoarthritis is the gradual wearing down of joint cartilage and narrowing of the joint space. It is a progressive condition most prevalent in individuals over 50 years old, although it can develop earlier after trauma. Patients typically report stiffness in the joint in the morning and pain that worsens with movement and improves with rest.
The degeneration of joint surfaces leads to restricted motion and reduced walking distance. For more detailed information on Symptoms and treatment of hip arthritis, please refer to our dedicated article.
Femoroacetabular Impingement (FAI)
Femoroacetabular Impingement (FAI) is a mechanical problem caused by a mismatch between the femoral head and the hip socket (acetabulum). It is especially common among young, active individuals and athletes. Structural bone overgrowth can cause impingement during hip movements, leading to cartilage and labrum damage.
Differences Between Arthritis and Impingement
Arthritis and impingement syndrome, two conditions often confused by patients, actually arise from different mechanisms. However, untreated impingement can eventually lead to arthritis. You can get more detailed information on Femoroacetabular impingement to better understand this distinction.
Onset Age and Risk Factors
Arthritis typically affects middle-aged and older individuals. Aging, obesity, and genetic predisposition are major risk factors. Conversely, FAI symptoms usually appear between ages 20 and 40, especially in sports that require excessive hip flexion like football, ice hockey, and martial arts.
Pain Type and Triggers
Arthritic pain is typically mechanical: it worsens with joint use and lessens with rest. Night pain may occur in later stages. Impingement pain is sharp and triggered by specific movements such as crossing the legs, getting out of a car, or deep squats. Prolonged sitting can also exacerbate the pain.
When Should You See a Doctor for Hip Pain?
Mild muscle pains usually improve with rest, but some signs may indicate a serious joint problem requiring prompt medical attention:
- Severe pain starting suddenly or after trauma,
- Inability to bear weight or limping,
- Pain that wakes you up at night,
- Swelling, redness, or warmth around the joint,
- Groin pain persisting despite several days of rest.
Diagnostic Methods
Accurate diagnosis begins with a detailed patient history and physical examination. The physician evaluates the range of motion and performs specific tests to provoke pain.
Imaging is essential to confirm the diagnosis. X-rays show bone structure and signs of arthritis, while MRI provides detailed images of soft tissues, cartilage damage, and labral tears. In some cases, joint-preserving surgery might be considered, and you can learn more about Osteotomy surgery indications.
Home Care Tips for Hip Pain
Until a diagnosis is made, or as advised by your doctor, the following methods may help alleviate pain but are not curative:
- Activity Modification: Avoid movements that worsen pain, such as deep squats and long walks.
- Weight Management: Reducing load on the joint.
- Cold Application: Use ice packs after activity to decrease pain and swelling.
In advanced cases or where surgery is necessary, home care alone may be insufficient. For example, arthroscopic surgery for Femoroacetabular impingement could be required. Additionally, regenerative medicine treatments like PRP therapy for the hip might be an option for suitable patients.
Commonly Confused Conditions: Sciatica or Hip Pain?
A frequent confusion arises between pain radiating from lumbar spine disorders and true hip joint pain. Sciatica typically originates from the lower back and radiates to the back of the hip and down the leg. True hip joint pain is mostly felt in the groin (inner thigh) area.
Distinguishing these two is critical as treatment plans differ significantly. For a detailed explanation, see Differentiating hip pain from sciatica.
Conclusion and Medical Disclaimer
Causes of hip pain vary according to the patient’s age, activity level, and pain characteristics. Arthritis and impingement syndrome are the most common causes, but accurate diagnosis can only be made by a specialist physician. Early diagnosis is essential to protect the hip joint and prevent or delay surgery. If your pain affects your quality of life, seeking professional evaluation is recommended.
The content provided is for informational purposes only and contains general medical information. Diagnosis and treatment should be determined by a qualified healthcare professional based on an individual examination. The information on this site is not a substitute for professional medical advice, diagnosis, or treatment. Please consult a licensed healthcare provider for any medical concerns and do not delay seeking necessary care.
FAQ
-
Where is hip pain most commonly felt?
Hip pain is usually felt in the groin (front), the outer side of the hip (trochanteric area), the front of the thigh, or the back of the hip (gluteal region). The location of pain gives important clues to the doctor about the underlying cause (whether it's inside or outside the joint).
-
What are the main differences between hip osteoarthritis and hip impingement (FAI)?
Hip osteoarthritis typically develops with age as the joint cartilage wears down, while hip impingement occurs in younger people due to structural mismatches in the bone (head-neck junction or socket). Osteoarthritis is characterized by morning stiffness, whereas impingement causes sharp pain during specific movements like bending or twisting.
-
When should hip pain be taken seriously and when should you see a doctor?
You should see a doctor if you experience severe, sudden hip pain that doesn’t improve with rest, wakes you at night, or is accompanied by neurological symptoms like numbness or weakness in the leg. If there is fever or redness, urgent evaluation is needed to rule out infection.
-
What can be done at home to relieve hip pain?
At home, rest, activity modification, applying ice or heat, and using over-the-counter pain relievers as advised by a doctor can help. However, self-treatment for a long time without a diagnosis is not recommended. If pain persists, consult a specialist.
-
What methods are used to diagnose hip pain?
Diagnosing hip pain involves a thorough physical exam, X-rays (for bone structures), MRI (for soft tissues and cartilage), and sometimes CT scans. Blood tests may be requested to rule out infections or rheumatic conditions if needed.